By Laura Brown
Forty-one-year-old Alice Isaacson had accomplished a lot by the time she joined the Canadian Army Medical Corps (CAMC) as part of the Canadian Expeditionary Force (CEF) in 1916. The Irish-born, American-trained nurse had eight years of nursing supervisor experience under her belt, as well as a year of service with the 23rd General Hospital of the British Expeditionary Force (BEF) in Étaples, France. A reference letter penned by a Medical Officer, likely in support of her transfer from the BEF to the CEF, described her as “skillful, energetic and reliable” and as an individual who was undaunted by large tasks. On one occasion she was responsible for looking after 120 seriously ill patients with little assistance. One of the few things she had not yet learned to do was ride a bicycle, but this, too, would be tackled with determination before her return home at the end of the war.
Alice kept several diaries during her service overseas, which included postings in France at the No. 2 Canadian General Hospital at Le Tréport and the No. 6 Canadian General Hospital at Troyes. Her writings and an insightful photo album are now part of her fonds held at Library and Archives Canada (LAC). These records, as well as other private and government collections, such as the Department of National Defence fonds, are some of the examples of the valuable archival resources at LAC that document the history of women’s service in Canada’s military.

Personnel riding bicycles, No. 6 Canadian General Hospital, Troyes, France, June 2, 1917. Photograph Album of Alice E. Isaacson, R11203-01-E (e002283123)
Only a few nurses were part of the Canadian Army Medical Corps at the start of the First World War in 1914, but numbers soon increased as civilian nurses were eager to transfer their skills into the military context. In total, more than 3,000 nurses served in the CAMC, including 2,504 overseas in England, France, and at Gallipoli, Alexandria and Salonika in the Eastern Mediterranean.
Nursing was the only means by which women were permitted to serve in the Canadian military during the First World War. To enlist, nurses had to be single, British subjects (which included Canadians at the time), in good health, between the ages of 21 and 38, and have qualifications from a recognized nursing school. If accepted, recruits were commissioned as officers with the rank of lieutenant, which is notable as Canada was the only country in the world to rate nurses as officers at the time. Canadian nurses were addressed with the traditional title of “Nursing Sister”, and enjoyed a number of benefits in their positions, including good wages and leave. The head nursing sister, known as the Matron-in-Chief, was in charge of all the nurses in the service. Margaret Macdonald of the CAMC was given this title, and was the first woman to hold the rank of major in the whole of the British Empire.

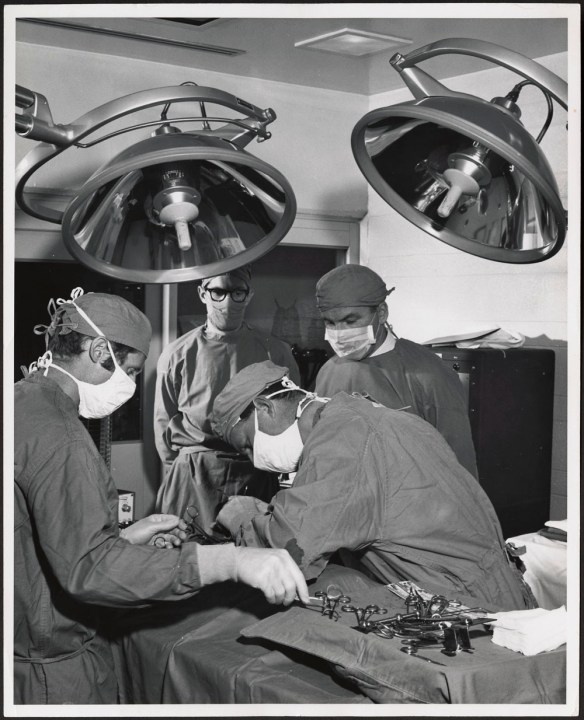
Nursing sisters attending to soldiers in a dressing tent at No. 7 Canadian General Hospital, Étaples, France, ca. 1917. W.L. Kidd Collection (e002712847)
Military nurses faced a multitude of new experiences that contrasted to their work in the civilian context, whether it was sleeping in a tent, shifting to a new posting at short notice, or making do with limited supplies. Improvising and adapting to changing circumstances was necessary, as nurses might face quiet wards with a few patients one day, and masses of incoming and outgoing patients the next. These women saw first-hand the bodily harm caused by the era’s modern warfare, including shrapnel and poison gas, and witnessed a loss of life that few could have predicted when they first enlisted.
Nurses were not permitted to serve in trenches and most were posted well back from the front lines, working in general or convalescent hospitals. However, some were tasked closer to enemy action. Alice Isaacson noted the coveted nursing positions at casualty clearing stations (advance units along the evacuation routes between front lines and hospitals) in her diary, while posted at No. 2 Canadian General Hospital in September 1917: “Such an exciting afternoon today! . . . Sisters Jean Johnston, S.P. Johnson and Riddle are to go to CCS tomorrow morning! Sisters Hally and Villeneuve are heartbroken at being left here – But we are all glad these sisters have their chance for CCS at last.”

Nursing Sister Lillias Morden with patients outside of a medical hut at No. 2 Canadian General Hospital, Le Tréport, France, 1917. Photograph Album of Alice E. Isaacson, R11203-01-E. (e007150684)
Nurses made significant contributions to the war effort in their care of ill and injured soldiers, a duty that extended after the armistice on November 11, 1918. The “Spanish flu” influenza pandemic that began at the end of the war and spread through military camps placed further demands on nurses. Close to 1,500 nursing sisters were still serving with the CAMC by mid-1919. Lillias Morden, a nurse from Hamilton, Ontario, was one of them. She joined the CAMC in 1916, served in England and France, and assisted with demobilization efforts at the end of the war. Morden did not leave her military position until November 1920.
While nurses such as Alice Isaacson and Lillias Morden made it home after the First World War ended, some nursing sisters were not as fortunate. Part II of this blog post will explore how the conditions under which nursing sisters served could be dangerous, with some paying the ultimate price.
Related resources
- Database: Personnel records of the First World War
- Examples of sources about nursing sisters that are in LAC’s collection and in other institutions can be found on LAC’s Nursing Sisters blog post (published July 23, 2015) and web page, The Call to Duty: Canada’s Nursing Sisters. Also check out one of LAC’s recent private acquisitions: Luella Blanche Lee fonds. Nursing Sister Lee served in hospitals in France and the United Kingdom during the First World War.
- “O” prefix, and “M” prefix are sub-sub-series under the Canadian War Records Office photographic Collection, which documents the activities of the CEF during the First World War. This rich photographic collection contains a variety of images related to nursing sisters, including accommodations, leisure activities, portraits, and funerals.
- Geneviève Allard’s “Caregiving on the Front: The Experience of Canadian Military Nurses During World War I” in On All Frontiers: Four Centuries of Canadian Nursing. Christina Bates, Dianne Dodd and Nicole Rousseau (eds.). Ottawa: University of Ottawa Press, 2005, p. 153–167 (Chapter 10).
- Cynthia Toman, Sister Soldiers of the Great War: The Nurses of the Canadian Army Medical Corps. Vancouver: UBC Press, 2016.
In April 2018, Library and Archives Canada launched Co-Lab, a new collaboration tool, for the public to contribute by transcribing, tagging and interacting with historical records. Now we are adding a new challenge: showcasing the personal files of some of Canada’s nursing sisters who served in the First World War. You can get started right away!
Laura Brown is a Military Archivist in the Government Archives Division.